
-
The History and Mythology of the Tooth Fairy
posted: Apr. 23, 2024.

-
Every Day is Earth Day
posted: Apr. 16, 2024.

-
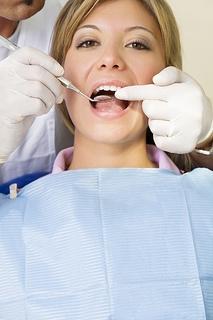
I haven’t been to the dentist in years; what should I expect?
posted: Apr. 09, 2024.
-
April is National Facial Protection Month
posted: Apr. 02, 2024.

-
What to Look for when Choosing a Mouthwash
posted: Mar. 26, 2024.

-
I’m on a diet and getting MORE cavities!
posted: Mar. 19, 2024.

-
Go Green for St. Patrick’s Day
posted: Mar. 12, 2024.

-
Good Nutrition Leads to Healthy Mouths
posted: Mar. 05, 2024.

-
Is a Crown Necessary for My Child’s Baby Tooth?
posted: Feb. 27, 2024.

-
Which whitening is right for you?
posted: Feb. 20, 2024.
-
Choose Chocolate on Valentine's Day
posted: Feb. 13, 2024.

-
Aging and Dental Health
posted: Feb. 06, 2024.

-
Oral Health Concerns Specific to Pregnant Women
posted: Jan. 30, 2024.

-
Seven Foods that will Give You a Smashing Smile
posted: Jan. 23, 2024.

-
Surprising Ways to Prevent Cavities
posted: Jan. 16, 2024.

-
Aging and Oral Health
posted: Jan. 09, 2024.

Contact Us
Send us an Email Today!
Featured Services
Click to find out more
Hours of Operation
Our Regular Schedule
Monday:
7:30 am-5:30 pm
Tuesday:
7:30 am-5:30 pm
Wednesday:
7:30 am-7:00 pm
Thursday:
7:30 am-5:30 pm
Friday:
8:00 am-1:00 pm
Saturday:
Closed
Sunday:
Closed
